DEFINITIONS:
inflammation – redness, swelling, and fever in any part of the body, often with pain
immune system – cells, cell products, and tissues that protects the body from infections, destroys infected and malignant cells, and removes damaged or dead cells
immunosuppressive medications – drugs that act on the immune system and decrease the number of cells that can damage patient’s tissues
Vasculitis is a disease that presents with the inflammation of the vessels. Its presentation is variable since it can damage small, medium or large vessels in different organs and tissues. Inflammation cause the vessel to become thickened, narrowed, or scarred. Damaged blood vessels can lead to decreased blood flow, abnormal organ work due to lack of blood flow, or bleeding secondary to rupture of the blood vessel. This damage can stay forever.
Most often, the cause of the vasculitis is unknown. Sometimes the cause can be identified (hepatitis B C, or HIV; drugs or other substances; another illness, such as lupus or rheumatoid arthritis).
CLASSIFICATION OF VASCULITIS:
1. Large vessel vasculitis: giant cell vasculitis, Takayasu’s disease
2. Medium vessel vasculitis: Kawasaki disease, polyarteritis nodosa (PAN)
3. Small vessel vasculitis:
a. ANCA associated vasculitis:
- microangiopathic polyangiitis (MPA)
- granulomatous polyangiitis (GPA, former Wegener’s)
- eosinopholic granulomatous polyangiitis (EGPA, former Churg-Strauss)
- anti-GBM
- cryoglobulinemic vasculitis
- IgA associated (former Henoch–Schönlein purpura)
c. Variable vessels:
- Behcet’s disease
- Cogan’s syndrome
d. Single organ vasculitis:
- central nervous system vasculitis
- hypersensitivity vasculitis
e. Vasculitidies with possible cause:
- hepatitis B
- hepatitis C
- HIV
VASCULITIS SYMPTOMS
Symptoms of vasculitis vary and depend on the type of vasculitis and location in the body. Some common symptoms include:
- Fatigue or weakness
- Fever
- Muscle and joint pain
- Lack of appetite and weight loss
- Stomach pain
- Kidney problems (bloody or dark-colored urine)
- Nerve problems (pins and needles, weakness, burning skin pain)
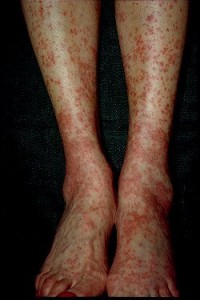
- Skin rashes or open sores
The tests used to diagnose vasculitis may include blood or urine tests, imaging tests (radiographs or MRI), special tests for nerve or lung function. A biopsy is often required to be sure of the diagnosis before starting treatment. Biopsy means taking a small piece of tissue to look under the microscope to make sure of the diagnosis.
VASCULITIS TREATMENT
It depends on the type of vasculitis. Treatment is usually continued until the disease is under control (called remission). The medications used for its treatment are:
- steroids (prednisone or methylprednisolone)
- immunosuppressive medications (cyclophosphamide, azathioprine, methotreaxate, mycophenolate mofetil)
- biologics (rituximab)
Sometimes prednisone is given through the mouth in large doses with following slow taper. Another steroid (methylprednisolone) can be given through the IV line and then switched to prednisone tablets.
Cyclophosphamide is one of the immunosuppressive medications used in the treatment of vasculitis. It is also called cytotoxic drug. It has dramatically improved the outlook for people with some types of vasculitis. It can be used along with steroids, and can be taken by mouth or can be given into a vein. Treatment is usually continued until the disease is under control (remission).
Hypersensitivity vasculitis (drug induced vasculitis) is treated differently than other types of vasculitis. In most people, stopping the medicine that caused the vasculitis is the only treatment needed.
See more under “Useful links” (vasculitis canada).